I have argued for some time that zero Covid is not a long-term sustainable strategy. It was undoubtedly the best policy for the first phase of the pandemic. The chart below shows the stark division in population mortality between countries that pursued elimination and those which did not. Hong Kong has done an excellent job at controlling the impact of the disease within our city. Despite understandable frustration with public health restrictions, it is important to not lose sight of the benefits of this policy so far. A resident of the USA, UK or EU is more than 70 times as likely to have died of Covid in the last two years than a resident of Hong Kong. In general Hong Kong has also avoided the lockdowns of much of the world. Notwithstanding frustrations around quarantine, school closures or mask mandates, all public health interventions are ultimately a balance between the costs of the disease in both human and economic terms and the costs of the public health measures to both the individual and the population.
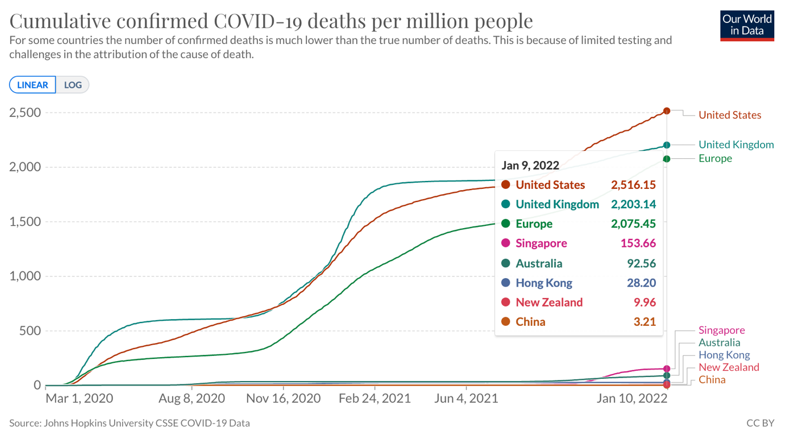
It is hard to argue against the success of elimination early in the pandemic. However, elimination was always a holding strategy, buying time to achieve high population immunity via vaccination. We have increasing evidence from South Africa, the UK, EU and recently from the USA,[1] that despite rapid surges of Covid the incidence of death and serious disease due to Omicron is significantly lower than from previous variants. All these countries have high levels of immunity from a combination of previous infections and vaccination. There is a suggestion that the impact of Omicron is greater in locations with lower levels of existing immunity. In this regard lessons from Singapore and Australia are very important. These countries, like Hong Kong, were essentially infection naive. So far the data provides reason to be cautiously optimistic that transition from zero Covid is possible without losing the historical population benefit. An exit wave and further deaths are likely whether or not the transition is planned or accidental. This point must be recognised and communicated. Not least because Hong Kong has an already overloaded health system, lower vaccination rates (especially in the most vulnerable) and more widespread use of less effective vaccines than Singapore or Australia. We will need to mitigate an evolving Omicron wave to a greater degree.
The recent outbreak of Omicron infections has changed the dynamic within our city. At this stage, at least in the short term, there are three possible scenarios.
-
- The fifth wave is controlled and we return to a Zero Covid strategy in Hong Kong
- Cases continue but public health restrictions are able to mitigate such that existing policies can continue.
- The rise in cases forces a strategic change.
1. Return to Zero Covid
Hong Kong has one of the best contact tracing systems in the world. However, the system of tracing all contacts of potentially infected individuals must by definition break down at relatively small daily numbers. We are now trying to trace contacts from people who have been in the community for days. In the context of our densely populated city and the highly transmissible nature of Omicron, it seems unlikely that we can now identify every potential touchpoint and return to zero cases.
2. Cases continue at a low level: continuation of the same strategy
The current policy of hospitalising all infective cases and quarantining all potential close contacts will inevitably be constrained by the number of hospital beds and quarantine facilities. Whilst it is possible to expand, at least quarantine facilities, this system will also break down at a relatively small daily case number. The greatest threat to the health system in Omicron waves is the need for healthcare workers to isolate when infected. Quarantining all healthcare workers who are contacts of infected cases will rapidly collapse the health system. Notwithstanding the public health and contact tracing expertise in Hong Kong, this scenario is unlikely to be sustainable.
3. Strategic Change
Ultimately living with Covid is the only sustainable long-term option. The challenge is to transition in such a way that the exit wave does minimal harm to the population. A key component of this strategy will be to drive high vaccination rates from the most vulnerable down whilst controlling case numbers below the level at which the health system can no longer cope. In Hong Kong this would mean that public health restrictions are likely to be in place for some time.
Omicron is highly transmissible. If the current outbreak is controlled it would represent an extraordinary achievement in terms of contact tracing and epidemiological control. We would then revert to our previous, longer term options:
-
- Continue with Zero Covid
- A planned exit once high vaccination rates have been achieved
What is the likeliest scenario?
Ultimately, the choice of non-pharmacological interventions aimed at risk reduction is influenced by the overriding strategy. Communication around zero Covid in Hong Kong has so far focused on the illusion of zero risk. Risk can never be eliminated, it can only ever be mitigated. One public health lesson for the future is that elimination strategies with a plan for exit and elimination strategies with no plan for exit are actually two different strategies. The latter encourages a focus on isolation and border control, it creates rational vaccine hesitancy and it shifts the risk-benefit and ethical justifications of both vaccination in low-risk groups and vaccine mandates. It also encourages negative messaging with a focus on blame. In pandemics public health communication should be positive, reliable and consistent, it should acknowledge uncertainty and be prepared to change on the basis of evolving evidence.
Frustration around contradictory and apparently irrational social distancing policies is natural. Media reports questioning the rationale of evening dining restrictions but not those earlier in the day and the recent closing of primary schools but not secondary schools, is an example of conflicted messaging. The reasons given for closing primary schools related to concerns about children being quarantined and the difficulties associated with respiratory infections in schools triggering covid testing. In other words, the justification did not relate to reducing transmission but rather mitigating complications of existing policy and managing resources. A rational public health response would be to either close all schools, to dampen transmission, or preferably keep schools open and focus on protecting and vaccinating the vulnerable. I have explained the rationale for social distancing in another article. Ultimately, social distancing measures are about reducing probability events. The government did not close beaches because of the risks on the beaches but because of the increasing touchpoints on public transport and in changing rooms. Of course every intervention has both a risk/benefit and also unintended consequences. In the case of closing beaches this may drive people into shopping malls and increase the actual risk. Social distancing regulations are metaphorically like taking balls off a snooker table to reduce the chances and probability of contact, especially mask off and/or protracted contact. The challenge is to control these touchpoints below the threshold at which infection rates challenge the health system. Ideally these nudges should have maximal benefit relative to their social and economic cost. School closures is one of the greatest challenges in this regard and any measure of risk must include the potential impact on the educational and social development of children.
We now have evidence of silent transmission chains within the community. The next two weeks should tell whether or not these chains can be controlled. Whilst it is reasonable to hope for the best, it is certainly rational to at least plan for a strategic shift towards mitigation, rather than elimination. Communication is currently focussed on the singular goal of Zero Covid. If this changes the transition is likely to be associated with mixed messaging, especially in the early stages. Over the next few weeks we are likely to see continued social distancing restrictions. Public health policy decisions, including school closures, will differ depending on whether the strategy is attempting to return to zero or mitigate the exit wave. I would be surprised if we do not eventually move away from hospitalisation of all positive infections and quarantine of close contacts and towards isolation of infected individuals at home. Social distancing measures will continue to be necessary in order to mitigate and flatten the exit wave. Whilst this would ideally have been actively managed later in the year, with the benefit of higher vaccination rates in the vulnerable, there is every reason to believe that an active mitigation strategy remains capable of preserving the majority of the benefit that accrued to Hong Kong as a result of early elimination.
Reference
1. Lewnard, J. A., Hong, V. X., Patel, M. M., Kahn, R., Lipsitch, M., & Tartof, S. Y. (2022, January 1). Clinical outcomes among patients infected with Omicron (B.1.1.529) SARS-CoV-2 variant in southern California. medRxiv. Retrieved January 13, 2022, from https://www.medrxiv.org/content/10.1101/2022.01.11.22269045v1
 Central General Practice
Central General Practice
 Repulse Bay
Repulse Bay
 Clearwater Bay
Clearwater Bay
 BodyWorX Clinic
BodyWorX Clinic
 Central Specialist Clinic
Central Specialist Clinic
 MindWorX Clinic
MindWorX Clinic
 Family Clinic
Family Clinic
 OT&P Annerley Midwives Clinic
OT&P Annerley Midwives Clinic
 WellWorX Clinic
WellWorX Clinic





