The short answer is that the increased infectivity of the newer variants and high vaccine hesitancy in Hong Kong makes it extremely unlikely that we can reach the Herd immunity threshold without any natural infection in our city. However, this may not be as important as some people think. The vaccines are incredibly effective on an individual basis. Herd immunity is not an all or nothing concept. Any level of immunity in the population will reduce the risks to our population. Obviously the more the better.
All infectious illness can be defined in terms of a basic reproduction number R0. This number is a measure of on average how many people are infected by an individual with the specific disease. If this number is <1 any individual will on average infect less than one other individual and the epidemic will die. If this number is >1 the epidemic is likely to grow. Infections with higher R0 values are more likely to spread. Population measures such as isolation of infected individuals, masks, hand washing, school closures, social distancing all work by reducing the exposure risk with the intention of reducing the effective transmission below 1 but regardless as much as possible in order to give the best possible chance for the epidemic to die.
Herd immunity is the point at which enough of the population are immune to an infectious disease that they provide indirect protection (herd immunity) to those who are not immune to the disease. The threshold for herd immunity is typically described by the formula:
1-1 / R0
For example, if an epidemic caused by an infectious disease has an R0 of 2, the average number of people an infected person goes on to infect is 2. Therefore, at least 50% (1-1/2) of the population needs to develop immunity for the disease to die out.
Of course things are never quite so simple. The effective immunity in a population is also impacted by the effectiveness of the vaccination. In this situation, the formula is A x B where A is the number of people vaccinated and B is the effectiveness of the vaccination that is given. So for example, if 90% of the population is vaccinated with a vaccine that is 90% effective the effective coverage would be 81%.
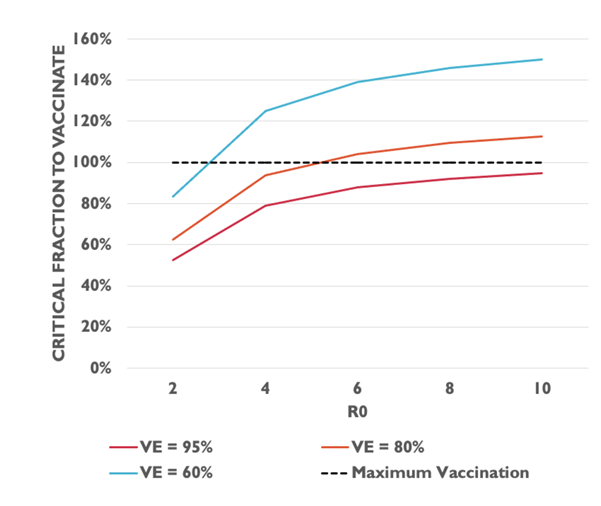
The graph above shows the percentage of the population that need to be vaccinated at different levels of R0 depending on how effective the vaccinations are (VE). BioNTech is closer to the red line (95%) whilst Sinovac is closer to the blue line (60%).
For COVID-19 the new variants have been shown to be more infectious. Initial modelling in Hong Kong early in the epidemic suggested the R0 to be around 2.4. More recently, with the new variants, R0 is considered to be between 4-8. This means between 75% (1-1/4 ) and 87.5% (1-1/8) of the population need to have immunity in order to for it to die out. The BioNTech vaccine has been shown to have effectiveness in excess of 90% although the evidence for Sinovac is closer to 50%. This suggests that even with very high vaccine uptake Hong Kong will struggle to achieve herd immunity.
Can Hong Kong reach Herd Immunity?
Countries that have had a mixture of high infection rate and high vaccine uptake will be the most likely to get herd immunity. The UK is probably at or very close to herd immunity. This has resulted from more than 60% population vaccination in addition to very high levels of infection. The low infection rate as a result of the public health measures, combined with the low vaccine uptake in Hong Kong suggests the levels of immunity will be way below the herd immunity threshold and the concept of herd immunity is still some way off. In Hong Kong, it is almost certainly not possible to get to herd immunity with vaccination alone. However, vaccines are extremely effective in protecting individuals. The higher the level of vaccine immunity, the less pressure there will be on hospitals and healthcare workers and restrictions can begin to be lifted. It is inevitable that some infections will occur in our city and it is especially important that we have high vaccination uptake in the most vulnerable. Zero covid is not a sustainable strategy. In the long term, it is inevitable that we will shift to a focus on high vaccination rates from the most vulnerable down. If we can achieve that, we will begin to transition to ‘living with covid’ which is the only feasible long-term strategy. A combination of some natural infections, reduced, intermittent public health measures and vaccination will allow life to return to normal.
 Central General Practice
Central General Practice
 Repulse Bay
Repulse Bay
 Clearwater Bay
Clearwater Bay
 BodyWorX Clinic
BodyWorX Clinic
 Central Specialist Clinic
Central Specialist Clinic
 MindWorX Clinic
MindWorX Clinic
 Family Clinic
Family Clinic
 OT&P Annerley Midwives Clinic
OT&P Annerley Midwives Clinic
 WellWorX Clinic
WellWorX Clinic





